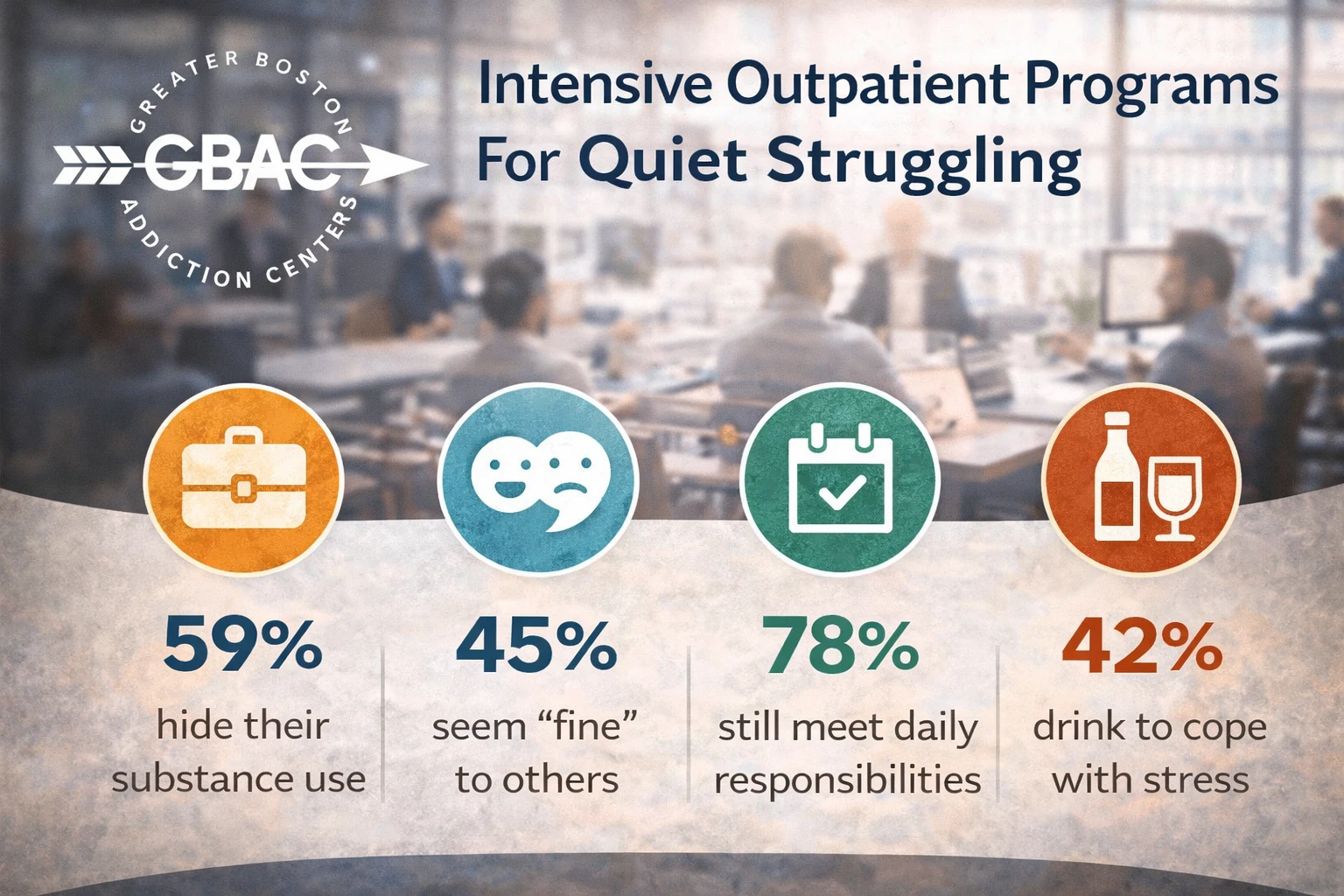
Why We Recommend an Intensive Outpatient Program to People Who Are Quietly Struggling
Clinically Reviewed by Dr. Kate Smith

You don’t have to hit bottom to ask for help. If you’re holding it together on the outside but breaking inside, an intensive outpatient program might be the step that saves your life—quietly, respectfully, and effectively.
You might be the kind of person who others describe as “strong,” “dependable,” or “the one who always handles it.” You show up every day, meet deadlines, take care of your responsibilities, and still manage to keep most people thinking you’re fine. But behind that composed exterior, there’s a part of you that feels like you’re barely staying afloat.
Maybe you’re drinking most evenings to calm a restless mind. Maybe you find yourself sneaking substances into your routine in ways no one else sees. Or maybe you tell yourself it’s not a problem because you still get to work, still make your deadlines, still love your family. If this feels familiar, you’re not alone—and you’re one of the people we think of first when we recommend an intensive outpatient program.
You don’t have to wait for a crisis to get help. You deserve help now.
What “Quiet Struggling” Really Feels Like
For people who are high‑functioning, struggling can be invisible to others—and incredibly loud inside.
Here are some of the thoughts we hear:
- “If I can still manage my life, it can’t be that bad.”
- “I’m not failing; I’m just coping.”
- “I’ll stop when it becomes a real problem.”
- “No one would understand; they think I’m fine.”
These thoughts can feel rational. They feel safe. They feel true. But there’s a hidden cost to keeping it all together while carrying a quiet desperation that no one sees.
You may be functioning on the outside, but the inside is where the real struggle lives—where the anxiety, shame, and exhaustion accumulate like invisible weight.
You might convince others you’re fine, but you know.
And deep down, you’re wondering if there’s a way to stop carrying all of this alone.
What an Intensive Outpatient Program Actually Is
An intensive outpatient program (IOP) is designed for people exactly like you:
- People with responsibilities
- People who can’t—or don’t want to—pause their whole life
- People who need structure, support, and real progress
- People who are still functioning but feel like something has to change
An IOP is not casual therapy. It’s not a weekly check‑in that you shrug off. It’s a structured, clinically supervised program that gives you the tools to navigate your life without relying on the very coping mechanisms that are slowly eating away at your wellbeing.
Most people in an IOP attend multiple sessions per week. These combine therapy, education, group support, relapse prevention, and skills training. But unlike residential treatment, participants return home at night. You maintain your job, your routines, your familiar world—but with professional support woven directly into your daily life.
This is why we recommend an intensive outpatient program to high‑functioning adults who are quietly struggling. It’s serious, but not disruptive. It’s clinically grounded, but still humane. It’s real help that fits into your life instead of ripping it apart.
When “Functioning” Becomes a Mask
Functioning doesn’t mean thriving. It means meeting expectations while your internal world is fraying.
Here’s what functioning often hides:
- Drinking to sleep, then waking up with dread
- Using substances to take the edge off anxiety, then needing more and more
- Avoiding conflict because confrontation drives you to cope in unhealthy ways
- Feeling numb, disconnected, or empty even when life “looks good”
- Hiding bottles, prescriptions, or habits so no one suspects
This is not resilience. This is survival with a cost.
One of the people we worked with recently described it like this: “I was living in two worlds. The world everyone saw—my job, my home, my routine. And the world no one saw—the late nights I couldn’t quiet, the things I told myself to justify it all.”
If this sounds like you—or someone you care about—it’s not denial. It’s fear. Fear of losing control. Fear of judgment. Fear of what treatment might mean for your identity.
But change doesn’t always come with drama. Sometimes it comes with honest acknowledgment that something needs to shift.
A Moment of Clarity: What It Feels Like on the Inside
People show up in treatment for all kinds of reasons:
- A quiet moment of panic after a night of drinking
- Realizing you’re relying on substances more than you want to
- Noticing your relationships are suffering
- Feeling like you’re living on autopilot
- Wondering why you feel stuck even when life looks “fine”
None of those reasons are small. None of them are excuses. And none of them mean you need to wait for a crisis before getting help.
We know someone who used to drive home from work and think, “Just one drink will calm me down.” That became two, then three, then a pattern he couldn’t control. But he still got up every day, fulfilled his job, and no one suspected a thing. Until one morning, he realized he couldn’t face the day without drinking first.
That moment of clarity—that it was no longer optional—is often what brings people to consider a structured program.
But imagine if he had support before it got to that point. That’s part of why we recommend an intensive outpatient program early—before things escalate, before the coping becomes dependence, before relationships start fracturing.
Who Benefits Most from an Intensive Outpatient Program
An IOP isn’t for everyone—but for many high‑functioning adults, it’s exactly the right step.
Here’s who typically benefits:
- People who are meeting daily responsibilities but struggling internally
- People who know they rely on substances longer than they want to
- People whose coping mechanisms are no longer working
- People who want support but can’t pause life to go residential
- People who want structure without uprooting everything
Even if you’re not sure you have a “clinical addiction,” if you’re asking yourself whether your use is problematic, that question alone is enough reason to explore help.
And it’s okay to seek help before a breaking point. In fact, prevention is strength.
What Happens in an IOP
You might picture treatment as an uncomfortable confessional or a cold clinical room with strangers who stare. But real, modern IOPs are different.
In an intensive outpatient program, you’ll likely experience:
- Individual therapy with a trained clinician
- Group therapy with peers who are also navigating challenges
- Education on coping skills, triggers, and emotional regulation
- Relapse prevention planning and real‑world skill building
- Support with stress, anxiety, and life management
Sessions are typically scheduled to allow you to keep your core responsibilities intact. Morning, evening, or flexible programming means you don’t have to choose between treatment and life.
Think of it as a guided reset. You’re not starting from scratch—you’re strengthening what’s already there.
A Real‑World Example That Isn’t Dramatic
One client came to us after months of telling himself he’d cut back “tomorrow.” He was known as reliable and charismatic. But he would pour drinks after work and tell himself, “This is just how I relax.” His wife noticed, but he minimized it. His kids didn’t know. His job was fine. On paper, nothing looked wrong.
But inside, he was overwhelmed:
“I couldn’t face life without a drink. If I didn’t take a break, I thought I’d fall apart.”
It took courage to say out loud, “I need help.”
He joined an IOP. Not residential. Not dramatic. Just a few hours a week, with real clinicians and real tools. Within a few weeks, he told us something surprising:
“I didn’t know how much I was surviving instead of living.”
That’s what treatment can do: it changes how you live, not just how you cope.
Why We Don’t Wait for Rock Bottom
There’s a myth that treatment is only for people who have hit rock bottom. That’s not true.
Most people who reach a point of crisis wish they had come for help earlier. Early intervention:
- Reduces harm
- Protects relationships
- Preserves careers
- Strengthens coping mechanisms
- Reduces long‑term psychological damage
An intensive outpatient program is not a last resort. It’s a powerful, proactive step toward lasting change.
Sometimes Struggle Isn’t Loud—It’s Quiet
Here’s something many high‑functioning people don’t realize: quiet struggle is still struggle.
And struggle, even when hidden, changes how you think, how you feel, and how you show up in the world.
You might be thinking:
“But I’m still handling things. I’m not out of control.”
That’s exactly why an IOP is appropriate. You don’t have to wait for chaos to act.
Getting help while you’re still functioning means you get your life back on terms you control—not terms dictated by crisis.
How Loved Ones See the Change
Sometimes loved ones know something is off before you do. They might say things like:
- “You’re not quite yourself.”
- “You seem tired all the time.”
- “I don’t want to nag, but I’m worried about you.”
Those comments aren’t judgment. They’re care.
If people around you are noticing changes, and you’re brushing them off, that’s usually a clue that something needs attention.
That’s where treatment becomes a gift—not just for you, but for the people who care about you.
And if someone has encouraged you to get help, that’s not weakness. It’s connection.
A Personal Note from the Clinician’s Chair
I’ve sat with people who could function better than most. Lawyers, teachers, parents, entrepreneurs, artists, caregivers. People who are used to solving problems.
None of them started treatment because something “dramatic” happened. They started because they realized the cost of coping was too high—and because they finally admitted to themselves that they deserved support.
There’s strength in that honesty.
There’s courage in saying, “I’m ready for help.”
And there’s real healing on the other side of that decision.
In some cases, people also explore other supportive treatment options like residential care, especially if deeper stabilization is needed. But for most high‑functioning adults, an intensive outpatient program is the right first step.
You don’t have to break down to begin. You can start right where you are—with intention, bravery, and support.
And if you want to take that step, we’re here to help.
Waltham, Massachusetts was once home to someone who thought treatment was only for people who had lost everything. Today, they tell others that seeking help was the best decision they ever made—long before life fell apart.
Frequently Asked Questions
What makes an intensive outpatient program different from regular therapy?
An IOP is more structured than weekly therapy. It includes multiple sessions per week, combines individual and group work, and focuses on comprehensive recovery skills rather than isolated talk therapy.
Do I need to stop working to join an IOP?
No. That’s one of the key benefits of an IOP. You can maintain your job, family life, and routines while attending scheduled treatment sessions.
Is an IOP only for people with severe addiction?
No. Many people who aren’t in crisis benefit from the structure and support of an IOP. It’s designed for those who are coping but feel their current strategies aren’t enough.
Will my employer find out?
Your privacy is protected. Treatment programs follow strict confidentiality rules. You choose what to share with others.
How long does an IOP last?
It varies based on individual needs, but most programs run several weeks with regular sessions. Your clinician will help determine the best duration for you.
Can I join an IOP if I’m unsure I have a problem?
Absolutely. If you’re questioning your patterns or feel that something needs to change, talking to a clinician and exploring options is a strong first step.
If you’re ready to explore meaningful change with professional support, Call (877) 920-6583 to learn more about our intensive outpatient program in Boston, Massachusetts.
Live Sober
Live Connected
Greater Boston Addiction Centers
Rehab Blog